Gut & Bowel Health
 Our nutritionists and dietitians firmly believe that a healthy digestive system generally leads to a healthy person. In fact, some of the most common health issues we see in recent times can be directly attributed to poor gut health and more broadly, dietary choices.
Our nutritionists and dietitians firmly believe that a healthy digestive system generally leads to a healthy person. In fact, some of the most common health issues we see in recent times can be directly attributed to poor gut health and more broadly, dietary choices.
Specialising in gut health and bowel health related disorders, we help hundreds of people in and around Brisbane each year with symptoms such as:
We love to talk about all things gut-related. Give us a call to arrange an appointment and let’s discuss your guts!
We can help improve your digestive health
Our team of experienced nutritionists and dietitians were specifically chosen and brought together to assist you in improving your digestive health. Using proven techniques culled from years of training, practice and experience, we create effective programs to relieve you of the symptoms associated with your condition, so that you are left feeling better from the inside out.
All our practitioners are accredited with the Dietitians Association of Australia, and have years of experience helping clients from all backgrounds with all types of medical conditions. Our combined knowledge and experience enables us to provide you with discrete, personalised and practical lifestyle solutions that are not only effective, but also easy to follow.
When you turn to Julie Masci or any of our professional nutritionists and dietitians, you get more than just a consultation. You are given the opportunity to work with a dedicated healthcare professional who will guide you as you make a change for a better you, and begin your journey to a healthier, happier life – a New Life. Not only will our team show you how to improve your health and general well-being, but we’ll also teach you how to boost your energy levels, improve your sleeping habits and increase your focus.
What is bowel & gut health? Why is it important?
You may have an idea of how your gut and bowels work, but you may not be aware of the issues that may arise if you ignore their impaired performance. Caring for your gut and bowels doesn’t just ensure the proper functioning of your gut and bowels– it also promotes the well-being of all areas of your body and good mental health. After all, your gut is connected to just about every other area of your body, your brain included.
Your gut and bowels – which make up your gastrointestinal system – are home to bacteria. For your gut to be healthy, there needs to be a balance of good and bad bacteria, both of which are always present within your gut. When your bacteria is balanced, all the other areas of your body flourish. But when your bacteria is out of balance, it can negatively impact everything from your body’s hormonal regulation to immune responses.
More recently, gastrointestinal health and moods have been closely linked, with researchers starting to label the gut as your body’s “second brain”. Your gastrointestinal tracts are lined with millions of nerve cells, and while one of its main functions is digestion, it is also responsible for communication between your gut and your brain. This is why people with conditions affecting their gut health, such as IBS or leaky gut, are more prone to certain mental health conditions, such as anxiety and depression.
An imbalance of bacteria in your gut can cause issues such as food intolerances or sensitivities, inflammation, and other diseases. Chronic inflammation of the gut has been known to impact mood and cognitive functions, once again leading to potential mental health difficulties.
A good balance, on the other hand, not only promotes physical health, but also mental well-being. The good bacteria within your gut can promote your brain health, improving everything from your memory function to focus. In essence, a happy gut is a happy brain – and ultimately, a happy person.
Our team of qualified nutritionists and dietitians are more than able and willing to help you improve your gut health. This might include testing for intolerance and diseases, recommending changes to your diet and lifestyle, and advising dietary supplements with the vitamins and minerals your body needs.
When you commit to making these lifestyle changes, you are not only boosting your bowel and gut health – you are also repairing and reversing the damage that’s already been done, making it a worthwhile option for anyone who wishes to live a healthier, happier life.
Bloating & Indigestion
Bloating and indigestion can be both painful and uncomfortable. Bloating occurs when your belly feels swollen after you have finished your meal. It is usually related to excessive gas production or muscle movement disturbances within your digestive system and brings a high degree of discomfort.
Indigestion usually presents itself as discomfort or pain within your upper abdomen, including a burning sensation behind your breastbone. Symptoms might appear on their own or together, causing greater discomfort. They usually arise right after you eat or drink, and is associated with feeling bloated or sick, belching or even regurgitating.
In most instances, indigestion is a mild condition that you don’t have to worry about. But when these flare-ups begin to occur on a regular basis, it’s worth looking at possible causes or lifestyle changes that could assist in eliminating or alleviating this problem.
Indigestion is sometimes caused by your stomach acid beginning to break down the lining of your stomach, called the mucosa. When this happens, your lining becomes inflamed and irritated, resulting in the pain you experience. In other instances, your mucosa simply becomes more sensitive.
Long term problems with bloating and indigestion can often be managed and alleviated with the right lifestyle changes. Book an appointment with our team of experienced practitioners now to discover a suitable treatment plan for you.
Excess Wind & Flatulence
Flatulence is the passing of gas from your digestive system and out through your anus. It is also known as “passing wind”. Everyone passes wind, but excessive flatulence can lead to your embarrassment and discomfort, as well as indicate underlying issues relating to your diet and lifestyle.
There is no “normal” amount to pass wind – some people do it around 5 times a day, others as many as 15 times a day. Passing wind happens when small pockets of air get transported into your digestive system when you eat and drink, or even when you swallow your own saliva. This gas begins to build up in your body and needs to be released somehow. This is done either through belching or passing wind.
Excessive flatulence is caused by eating foods that your body finds difficult to digest, or by consuming more air than usual when eating a meal. It can also be related to other, underlying health conditions, such as IBS.
There are a variety of ways to tackle this problem, including avoiding foods that you know causes gas build-up, or eating and drinking more slowly. Increasing your exercise or the regularity of your meals could also aid in reducing the problem.
Stomach Ulcers & Gastritis
Stomach ulcers occur when painful sores form in the stomach lining. This condition can lead to serious complications such as stomach bleeding or a hole in your stomach.
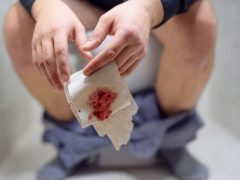
The most common symptom of a stomach ulcer is intense pain in the stomach between your breastbone and belly button. This pain often occurs when your stomach is empty, but it can also strike any time. Other symptoms of stomach ulcers include anaemia, weight loss, loss of appetite, bloody or black stool, vomiting with or without blood, and an upset stomach.
The Helicobacter pylori (H. pylori) bacteria and frequent use of non-steroidal anti-inflammatory drugs (NSAIDs, a type of pain killer) are the major causes of stomach ulcers. Antibiotics and lifestyle modifications such as quitting smoking are among the treatment options for stomach ulcers. More serious cases may require surgery.
Gastritis refers to an inflammation of your stomach lining. Acute gastritis comes and goes quickly, but chronic gastritis can persist for months or years. Complications include stomach ulcer, peptic ulcers that can lead to a bleeding ulcer, anaemia, gastric cancer, MALT lymphoma, renal issues, strictures, and bowel obstruction.
Some individuals who have gastritis show no symptoms. However, those who have either acute or chronic gastritis may experience abdominal pain, nausea, and vomiting. They may also suffer from belching, bloating, loss of appetite, and indigestion.
The H. pylori bacteria and repeated use of NSAIDs are the common causes of gastritis. Other possible causes include smoking, excessive consumption of alcohol or cocaine, stress, infectious agents, autoimmune issues, Crohn’s disease, sarcoidosis, and isolated granulomatous gastritis.
Treatment options for gastritis include antacids, histamine 2 (H2) blockers, and proton pump inhibitors (PPIs). Lifestyle modifications such as eating smaller and frequent meals, avoiding spicy foods, limiting alcohol intake, quitting smoking, and managing stress can help ease gastritis.
Diarrhoea & Constipation
Diarrhoea and constipation aren’t topics that are discussed very often, but they are very common conditions that affect a wide range of people. Understanding their causes and triggers can help you to avoid them.
Diarrhoea occurs when your stools are very loose, watery or runny. When it happens infrequently, diarrhoea isn’t damaging to your health, but frequent episodes could result in dehydration, which could lead to more serious health problems.
Diarrhoea may be caused by bacterial infections or viruses, or triggered by chronic conditions, such as IBS. Appropriate hygiene is often enough to stave off most cases of diarrhoea, such as washing your hands on a regular basis, especially before you eat or handle food.
Constipation occurs when your stool becomes difficult to pass. After your bowel movement, you will notice that your stool is often hard and small.
Proper diet is an important factor to prevent constipation, including reducing your caffeine, dairy and alcohol consumption. It is important to note, however, that constipation is not always diet-related. There is a range of health conditions that can cause it, including pregnancy, diabetes, IBS and hypothyroidism.
Infrequent cases of constipation usually clear up on their own but if you struggle with chronic constipation, you may want to consult with our qualified team of practitioners to better tackle this issue.
Haemorrhoids
Haemorrhoids are veins that have swelled within your anus and lower rectum. They are very common. They might arise due to straining during bowel movements, or from the increased pressure on the veins within the anus during pregnancy.
Depending on their location, haemorrhoids can be classified as internal haemorrhoids (within your rectum) or external haemorrhoids (outside your rectum). In many instances, they don’t cause extreme discomfort and often disappear on their own. In some instances, however, a clot can form within the haemorrhoid, causing a thrombosed haemorrhoid that can be quite painful.
Some of the more common symptoms of haemorrhoids include painless bleeding during bowel movements, itching, swelling around the areas of the anus and a lump near the anus.
In many instances, simple lifestyle changes can provide great relief and even prevent haemorrhoids from returning. Keeping your stool soft is the simplest way to prevent haemorrhoids. This can be accomplished through proper diet, enough water intake and exercise. Other preventive measures include going to the toilet when you feel the urge and not sitting for very prolonged periods of time.
Irritable Bowel Syndrome (IBS)
Irritable Bowel Syndrome, or IBS, is a condition that affects your large intestines. Different people experience its symptoms differently. For some people, the signs of IBS could centre around abdominal pain and bloating, while others could experience diarrhoea, constipation or both. For most people, Irritable Bowel Syndrome will remain a chronic condition that they will need to manage on a long-term basis. The good news is that it can be managed.
While there are some people who will struggle with severe IBS symptoms, most will not. These individuals will be able to manage the condition through dietary and lifestyle changes, as well as through stress management. Those with more severe symptoms might require additional support in managing their condition.
In most instances, those with IBS will experience episodes when their symptoms are worse, and when they are more manageable. While the causes of the condition remain unknown, there are a variety of contributing factors, including muscle contractions within your intestines, abnormalities within your nervous system, inflammation, infection and bacterial changes within your gut.
You might find that the symptoms of your IBS are worse when you eat certain foods or during periods of increased stress. Hormones might also play a large role – women are more likely to struggle with this condition than men.
Coeliac Disease
Coeliac Disease is a genetic, autoimmune disease that causes severe damage to your small intestine. Its symptoms include diarrhoea, constipation, gas, bloating, and abdominal pain. This disease can potentially result in nutrient malabsorption and malnutrition if left untreated. In more advanced cases, it may even lead to osteoporosis, cancer, and other serious health conditions.
Because coeliac disease shares most of the symptoms of Irritable Bowel Syndrome (IBS), it often goes undetected or misdiagnosed. In fact, approximately one out of 100 Australians have coeliac disease, but only an estimated 20% of this number have been diagnosed. That means around 80% of Australians are suffering from coeliac disease and are not even aware of it.
Individuals with coeliac disease are better off avoiding foods that contain gluten, which is a type of protein found in grains like wheat, rye, and barley. Their immune system perceives gluten as a harmful substance and releases antibodies that attack gluten once it reaches the small intestine. In the process, these antibodies end up damaging the villi, which are the finger-like projections along the intestinal lining that are responsible for nutrient absorption. This reaction triggers the symptoms mentioned earlier.
Since a cure for coeliac disease has yet to be discovered, the best way to manage this condition is to seek the help of a qualified dietitian who can help you develop a customised gluten-free diet that still meets your daily nutritional needs.
Crohn’s Disease
Crohn’s Disease is an IBD, or inflammatory bowel disease, that leads to chronic inflammation of your digestive tract. This leads to abdominal pain, fatigue, diarrhoea, malnutrition and weight loss, among other issues. It’s important to remember that Crohn’s disease can affect different parts of your digestive tract in a different way from other people who have the same condition.
The inflammation caused by Crohn’s disease can spread deep into your bowel tissue and be life-threatening in some instances. The symptoms themselves can be mild or severe but they aren’t present all the time. In most cases, they will appear during flare-ups, when the symptoms of the condition become very pronounced.
At present, there is no known cause of the condition, however, a range of factors seem to play a role in its development, including a weak immune system and genetics. There is also no known cure for Crohn’s disease, but it can be managed by lifestyle and dietary changes.
If you have been diagnosed with Crohn’s disease, it’s important to learn how the disease affects you and how you can best manage it. What works for one person might not work for others, so treatment plans need to be tailored to the individual patient. Our qualified team understands this well and specialises in providing personalised health solutions to all our clients. Book an appointment with us today so we can help you manage your health conditions in the best possible way.
Ulcerative Colitis
Ulcerative Colitis is a chronic condition that causes inflammation to your rectum and colon. Over time, ulcers can begin to form within the lining of your colon, and when they are irritated, they can bleed or even produce pus.
If you are struggling with ulcerative colitis, you will experience a range of symptoms, including chronic diarrhoea, abdominal pain and the urge to move your bowels on a more regular basis. In some instances, you might experience fatigue, a loss of appetite and even weight loss. The type of symptoms experienced, as well as their severity, will depend on the extent of your inflammation.
As a chronic condition, its symptoms arise time and time again, with occurrences of very mild symptoms at times and more severe, debilitating symptoms at other times. In many instances, you might experience symptoms in other areas of your body, such as mouth ulcers, irritated eyes and painful joints.
Professionals believe that this condition is an autoimmune problem, however, the exact cause isn’t known. It is believed that a combination of environmental and genetic factors could lead to the condition. While many flare-ups can be treated and managed at home, in more severe instances, hospital admission might be required.
FODMAPs
FODMAPs are essentially a short-chain carbohydrate, including fructose, sugar alcohols and lactose, among others. These can be found in a wide range of foods, such as wheat, certain fruits and vegetables, yoghurt, milk, soft cheeses and honey. The term FODMAP stands for Fermentable Oligo-, Di-, Mono-saccharides and Polyols (1).
You may have heard about the low FODMAPs diet if you have been diagnosed with IBS or other gut, bowel or digestive issues. This particular diet calls for your reduced intake of certain types of carbohydrates for periods of time to determine whether they reduce or eliminate your symptoms.
The reason low FODMAP diets are becoming more and more popular is because these types of foods are well known for causing a range of digestive issues, including gas, bloating, diarrhoea and stomach pain, among other problems. The human body often finds these foods difficult to digest, causing the range of negative symptoms to appear.
Determining whether you have a FODMAP sensitivity will take some time. It requires us to focus on the impact of what you eat, even days after you have consumed these products as some reactions can be delayed for hours or even days.
Ready for a healthier life? Book an appointment now.
At New Life Nutrition, we take pride in having earned reputable, professional certifications in our respective industries. We come from different backgrounds but we are all united by our common goal to help you change the way you approach food and nutrition. We are committed to help you change the way you eat now, so you can change the way you feel forever.
Call us now at (07) 3071 7405 to book an appointment and speak to our qualified nutritionists and dietitians.